Emery Haley, PhD, Scientific Writing Specialist
Viridans Group Streptococci [Streptococcus anginosus, Streptococcus oralis, and Streptococcus gallolyticus subspecies pasteuranus]
Clinical Summary
- Viridans Group Streptococci (VGS) are nitrite-negative, biofilm-forming, gram-positive microorganisms.
- VGS are commonly dismissed as contaminants in standard urine culture conditions.
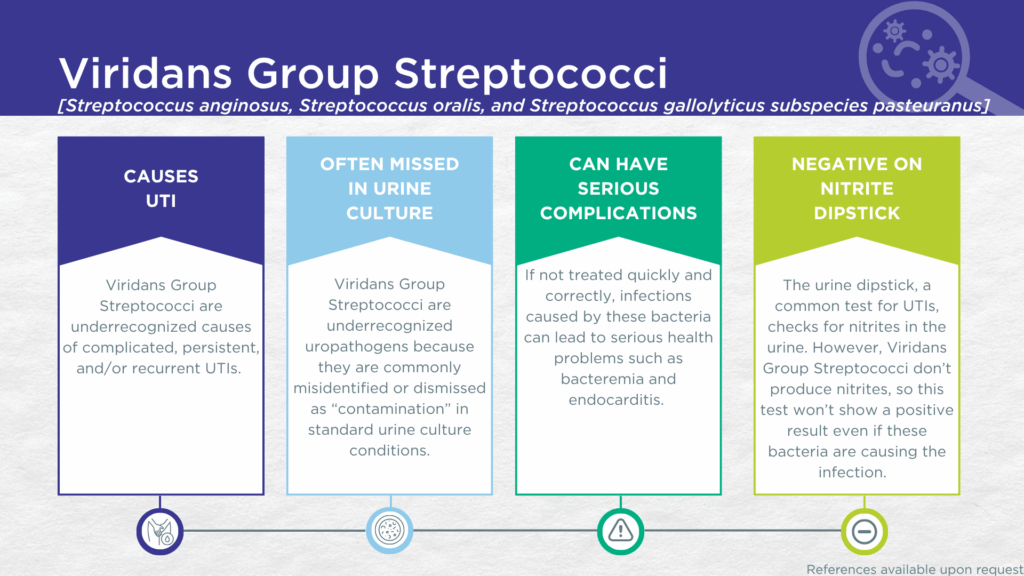
- VGS are associated with complicated, persistent, and/or recurrent UTIs.
- In symptomatic UTI patients, VGS:
- Are not contaminants (are found in catheter-collected urine specimens).
- Are viable (can grow out on culture).
- Are pathogenic (associated with elevated urine biomarkers of infection).
- Reported severe complications of VGS UTI include bacteremia and endocarditis.
Bacterial Characteristics
Gram-stain
Gram-positive (all)
Morphology
Coccus (all)
Growth Requirements
Non-fastidious (all grow well in standard urine culture conditions)
- S. anginosus is a microaerophile
- S. oralis and S. pasteuranus are facultative anaerobes
*Note: We do not perform P-AST™ on Streptococci (including Viridans Group Streptococci). Streptococci have well-established and predictably high susceptibilities to beta-lactam antibiotics, particularly penicillin and ampicillin (see treatment section). Therefore, confirmation of susceptibility by P-AST™ assay is unnecessary.
Nitrate Reduction
No (except S. oralis is variable for this phenotype)
Urease
Negative (all)
Biofilm Formation
Yes (all)
Pathogenicity
Colonizer or Pathobiont
Clinical Relevance in UTI
Viridans Group Streptococci (VGS) is a historic pseudo-taxonomic term for several Streptococcus species traditionally described as gram-positive commensals of the human microbiome.[1] In the Guidance® UTI assay, this group term specifically encompasses three species, S. anginosus, S. oralis, and S. pasteuranus.
S. anginosus
The best-studied of these species, S. anginosus, was first described in 1906.[2] Genetic sequencing studies have confirmed that virtually identical strains of S. anginosus are present in both the vagina and bladder of same subject,[3,4] consistent with the reported interactions between vaginal and urinary microbiomes.[3,5] S. anginosus, has been identified by expanded quantitative urine culture (EQUC) in catheter-obtained urine specimens from women with various lower urinary tract disorders, including interstitial cystitis/bladder pain syndrome (IC/BPS),[6] and UTI,[8–10] at higher densities and with higher frequency than among asymptomatic women. These findings suggest that S. anginosus is involved in dysbiosis of urogenital microbiomes and may act as an opportunistic uropathogen.[11] Indeed S. anginosus is known to act as an opportunistic uropathogen at other body sites in immune compromised individuals.[12] S. anginosus has also been associated with recurrent UTI,[13,14] and with severe complications including bacteremia[15] and endocarditis[16,17].
S. oralis
Though less well studied, S. oralis (part of the S. mitis subgroup of VGS) has also been associated with urogenital microbiome dysbiosis[18] and complicated UTI, particularly in immune compromised individuals[19–22] . S. oralis UTI may lead to severe complications including bacteremia,[22,23] peritonitis,[22,24] endocarditis,[22,25] and meningitis[22,26] .
S. pasteuranus
Though less well studied, S. pasteuranus (part of the S. bovis subgroup of VGS) has also been associated with complicated, persistent, and recurrent UTI, particularly in neonates, older adults, pregnant women, and immune compromised individuals.[27–31] S. pasteuranus UTI may lead to severe complications including bacteremia,[29,31] endocarditis,[30] meningitis,[32] and sepsis[32].
The Viridans Streptococci Group
VGS UTIs are likely significantly underdiagnosed for a couple of reasons. Firstly, VGS organisms generally lack nitrate reductase activity, so screening strategies involving urinalysis for nitrite positivity will be false-negative.[33,34] Secondly, although the organisms grow readily in standard urine culture conditions, they are commonly dismissed as irrelevant gram-positive commensal organisms of the urogenital microbiome and labeled as a “contaminant”. [1]
However, in a study of older adult males and females with clinically suspected complicated UTI, VGS was detected in both midstream voided and in-and-out-catheter collected specimens indicating that it was truly present in the bladder, not simply a contaminant picked up during voiding.[35] Furthermore, elevated markers of immune system activation in the urinary tract have been measured from the same clinical urine specimens in which VGS was detected, indicating that the presence of VGS was associated with an immune response to urinary tract infection.[36–38]
Despite their reputation as contaminants, VGS (S. anginosus, S. oralis, and S. pasteuranus) are all associated with complicated, persistent, and/or recurrent UTIs, as well as with severe complications such as bacteremia and endocarditis. Together, these findings indicate that VGS should be seriously considered as a uropathogen and demonstrate the value of detecting these organisms, particularly in individuals with immune compromise or other risk factors for complicated, persistent, or recurrent UTI.
Treatment
Evidence of Efficacy (Checkmarks): Ampicillin, Cefepime, Ceftriaxone, Levofloxacin, Linezolid, Meropenem, and Vancomycin.
Because Streptococci have well-established and predictably high susceptibilities to beta-lactam antibiotics, confirmation of susceptibility by P-AST™ assay is unnecessary. To provide faster result reporting without compromising relevant treatment options, Pathnostics provides a report without P-AST™ for monomicrobial Streptococci. See the checkmarks for suggested treatment options.


